E-Learning & Technology The Virtual Longitudinal Curriculum Model Welcome to the future! The 2021 SACME Annual Meeting is going virtual. Therefore, SACME formed the Virtual Meeting Task Force to explore the pros and cons of three distinctly different curriculum/conference models:
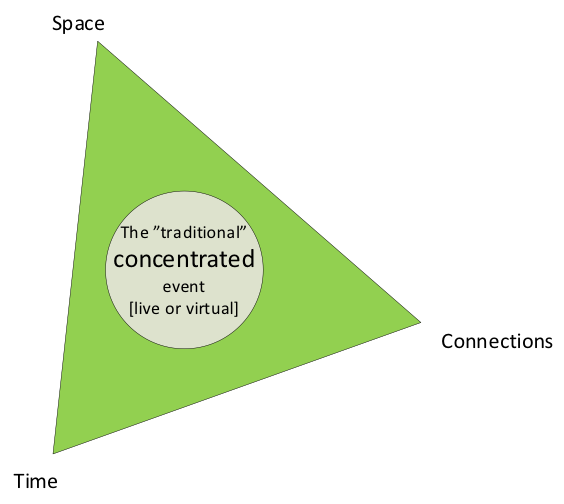
For this first article in E-learning and Technology, I will focus solely on a discussion of the longitudinal curriculum/conference model. As we were discussing the reasoning for the longitudinal delivery format, Morag Paton, a member of our workgroup, framed the key question: Can we put the "continuing" back into continuing professional development in the context of a traditional annual meeting? This is, indeed, a big question. Let me explain. The traditional annual meeting model is limited to a specific time and space. It is not continuous. That seemingly small detail has a lasting impact. We can all recall coming back from annual meetings full of great ideas and ambitions to improve our practice. Yet, it is hard to realize those ambitions. Sometimes we share our improvement plans with a co-worker or two. But, very often, we continue practicing just the same as before. The main building block behind those challenges is that there is a time and space gap between the annual meeting and our professional practice. This is where the longitudinal meeting model comes in. The longitudinal model is about extending the traditional annual meeting and making it more continuous. The extended meeting can last from a few weeks to a few months. We are doing that extension in three dimensions, as this image illustrates: Time, Space, and Connections. Figure 1. Extending the traditional meeting in 3 dimensions
Those benefits are well documented. Austin, Carney, Thayer, and Rozansky (2019) provide a convincing story of how active learning and sequencing learning modalities can enhance CME/GME conferences and foster the creation of a vibrant learning community of practice. Margolis, Balmer, Zimmerman, and López-Arredondo (2020) provide proof of concept on the international stage. Their paper is a captivating story of 774 participants from 20 countries learning together as a community of practice and each simultaneously improving his or her own unique local practice. Finally, the well-known findings of Cervero and Gaines (2015) send a strong message about how the longitudinal annual meeting formatting should look. Impactful CME/CPD "is more interactive, uses more methods, involves multiple exposures, is longer, and is focused on outcomes that are considered necessary by physicians’’ (p. 136). Kolb's experiential learning theory (Kolb, 2015) explains benefits of the longitudinal model. Kolb's model describes learning as a continuous cyclical process that goes through four phases: (1) abstract conceptualization, (2) active experimentation, (3) concrete experience, and (4) reflective observation. The traditional meeting effectively addresses the first stage of that cycle – abstract conceptualization. For example, listening to discussions about research (abstracts) during an annual meeting is the abstract conceptualization. We are trying to conceptualize new ideas in abstract form. That part is done well. Unfortunately, the other three elements of Kolb’s cycle cannot be adequately addressed by traditional annual meeting formatting. This is where longitudinal, technology-enhanced meetings can make a big difference. With the longitudinal meeting, we have the time and tools for active experimentation. We have significantly more time to discuss ideas with peers, create project plans, use role-play, and employ peer assessment. To better address the schedules of busy professionals, almost all these activities can be done in an asynchronous format. Then we can implement some of those ideas in our local context. Here, learning is connected with our professional practice. Finally, we have time and space for reflection. We can share with our local organization and our learning peers the improvements we made and the lessons we learned. Many institutions are struggling to provide meaningful faculty development training, especially in the domains of teaching skills, learner assessment and evaluation, among others. Typically, this kind of training curriculum involves didactic lecture (abstract concepts in adult learning principles and strategies), applied, “hands-on” training, deployment to various teaching settings, and measurement of effectiveness via improved learner outcomes. A longitudinal curriculum model can provide an experiential experience in all phases of learning in satisfaction of Kolb’s complete cycle. In exhibit 1 below, envisioned by Robert Dantuono, a member of our Longitudinal Workgroup, an institution has developed an intensive faculty development curriculum to improve faculty skills in the basics of clinical teaching, learner assessment and evaluation. The core curriculum sessions last 5 weeks and then continues with an extended period to complete a capstone project. Week 1 is an orientation week with sessions devoted to assuring that all participants are familiar with the virtual environment tools and other resources of the meeting platform. Also in Week 1, a “flipped classroom” session will begin the curriculum. Learners must complete an on-demand lecture on Adult Learning Principles and Strategies for Medical Education, required readings and successfully complete a written post-test. A discussion board will be started whereby learners can discuss readings and share insights. Exhibit 1
In Weeks 2, 3 and 4 the faculty development curriculum will begin with a series of “core” lectures listed in exhibit 2. Each week, up to 3, ninety-minute sessions will be scheduled. Each session will include a synchronous core 30-35 minute didactic lecture and video, immediately followed by a 60-minute synchronous session whereby learners will break-out into small work groups for discussion and to complete guided exercises. Case studies will be presented for analysis and discussion as will self-assessment tools. Role-playing will be used to practice teaching tools as well as feedback and evaluation tools. A discussion board will be available to document key discussion points and learnings. Faculty will serve as facilitators of the small group sessions. Each session will end with a report out and review of major points. Exhibit 2
In Week 5, a wrap-up session is planned for learners to discuss requirements of the Capstone Project. Learners will be given an additional 4 months 1) develop a capstone project topic, goals and research methodology; 2) establish their institutional project teams; and 3) implement the project, observe and record outcomes. During this period of research, learners will have access to learner chat rooms, scheduled faculty “office hours” for guided assistance. Additional “on-demand” content presentations as needed. At the end of 4 months, learners will record a video presentation of their project, experiences, outcomes and lessons learned. Faculty will assess the projects for achievement of stated criteria and award a certificate accordingly. With a longitudinal model, we can undergo all of Kolb's cycle. When Kolb's Wheel is running/rotating, we will ideally use it for many follow-up activities. If the wheel is rotating – do not slow down. Make it run faster! Vjekoslav Hlede, PhD is a Senior Learning Management Specialist with the American Society of Anesthesiologists, Chicago. References Austin, J. P., Carney, P. A., Thayer, E. K., & Rozansky, D. J. (2019). Use of Active Learning and Sequencing in a Weekly Continuing Medical Education/Graduate Medical Education Conference. Journal of Continuing Education in the Health Professions, 39(2), 136-143. doi:https://doi.org/10.1097/ceh.0000000000000247 Cervero, R. M., & Gaines, J. K. (2015). The Impact of CME on Physician Performance and Patient Health Outcomes: An Updated Synthesis of Systematic Reviews. Journal of Continuing Education in the Health Professions, 35(2), 131-138. doi:https://doi.org/10.1002/chp.21290 Kolb, D. A. (2015). Experiential Learning: Experience as the Source of Learning and Development. USA: Pearson Education Limited. Margolis, A., Balmer, J. T., Zimmerman, A., & López-Arredondo, A. (2020). The Extended Congress: Reimagining scientific meetings after the COVID-19 pandemic. MedEdPublish, 9(128). doi:https://doi.org/10.15694/mep.2020.000128.1 |
Explore more from CE News archive | Fall 2020
Feature Article Leadership Publications and Scholarship European CME/CPD Canadian CME/CPD Funding Opps Events

 T
T